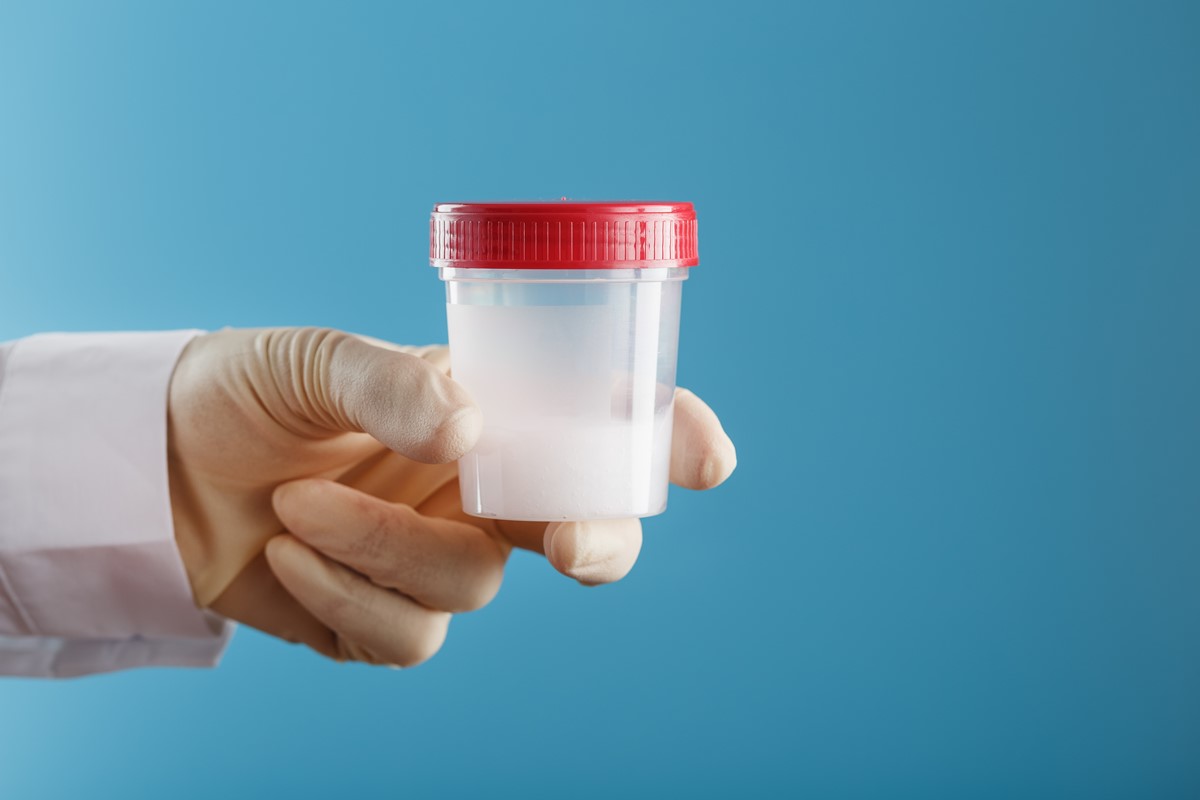
The entire process of human spermatogenesis can vary in length, but previous studies estimate it at 42–76 days. The mid-piece of the spermatozoa contains abundant mitochondria to produce ATP production that provides energy for the sperm cell’s flagellum, or tail, which allows for propulsion. The head contains the nucleus and is covered by the acrosome, which is filled with lysosomes that assist in fusion with an ovum. 
A fully mature sperm cell consists of a head, midpiece, and tail. After immotile spermatozoa are released into the tubules, they travel to the epididymis for further maturation and the development of functional motility. Furthermore, the exact number of stages of spermatogenesis remains unclear and debated. Once puberty has begun, one cycle of spermatogenesis within the Sertoli cell epithelia begins every 13–16 days however, spermatogenesis is not consistently synchronous throughout all seminiferous tubules. 
Sertoli cells, stimulated by follicle-stimulating hormone (FSH), and Leydig Cells, stimulated by luteinizing hormone (LH), both help to regulate spermatogenesis. The development of spermatozoa, a process known as spermatogenesis, begins at puberty with mature spermatozoa originating from germ cells found within the basement membrane of the seminiferous tubules of the testes. Numerous factors that determine the fraction of spermatozoa in semen have been studied, including metabolic syndromes (e.g., diabetes mellitus), diet, drug use, varicoceles, outflow tract obstructing pathologies, and various genetic pathologies such as Klinefelter syndrome. As such, only a small fraction of the semen is composed of spermatozoa. However, approximately 90% of the semen is composed of fluid from the seminal vesicles, prostate, and bulbourethral gland, in descending order of percent contribution. The composition of post-ejaculatory semen is highly variable between men and within individual men over the course of their lifetimes. In doing so, we aim to create a resource that providers and patients may reference when abnormalities in these characteristics are encountered. This will be followed by a detailed literature review exploring the etiologies, significance, and management, when available, of variances in the macroscopic characteristics of SA. In this article, we will briefly review the normal physiology of semen formation and ejaculation. A better understanding of these variables has important clinical implications for medical providers but would also empower patients with a knowledge of normal and abnormal semen variances. However, a paucity of literature exists regarding abnormal macroscopic features of SA, including semen volume, viscosity, liquefaction, pH, and appearance or color. Many components of SA have been thoroughly explored, including a modern review of conventional methods and clinical interpretation of variables. 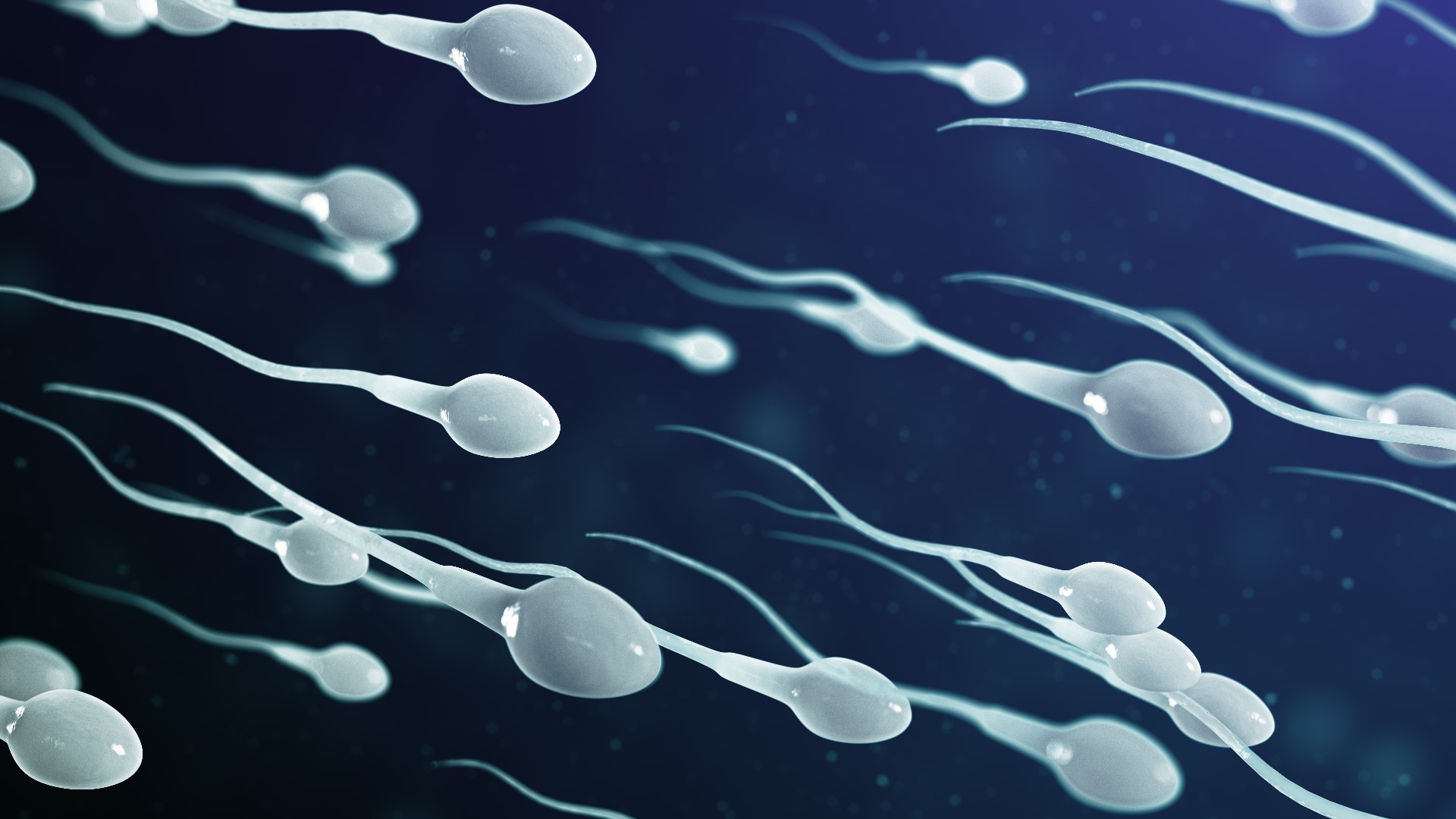
Results are also widely variable depending on sample collection methods, length of abstinence, and other factors. Although SA is considered the gold standard of male fertility assessment, this test has been shown to be a poor indicator of reproductive outcomes. Beyond fertility implications, an abnormal SA has been associated with higher rates of testicular cancer and multiple non-malignant chronic diseases. This test includes an assessment of macroscopic and microscopic parameters through a series of tests as described by the World Health Organization (WHO). Semen analysis (SA) has long been the first investigative tool used when assessing the male factor in couples with infertility, which is a contributing factor in approximately 50% of cases. Human male ejaculate, or semen, is an organic mixture composed of spermatozoa and fluid from the seminal vesicles, prostate, and bulbourethral glands.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
